Journal Series to Explore Integration Science as Key to Meeting Global Health Challenges
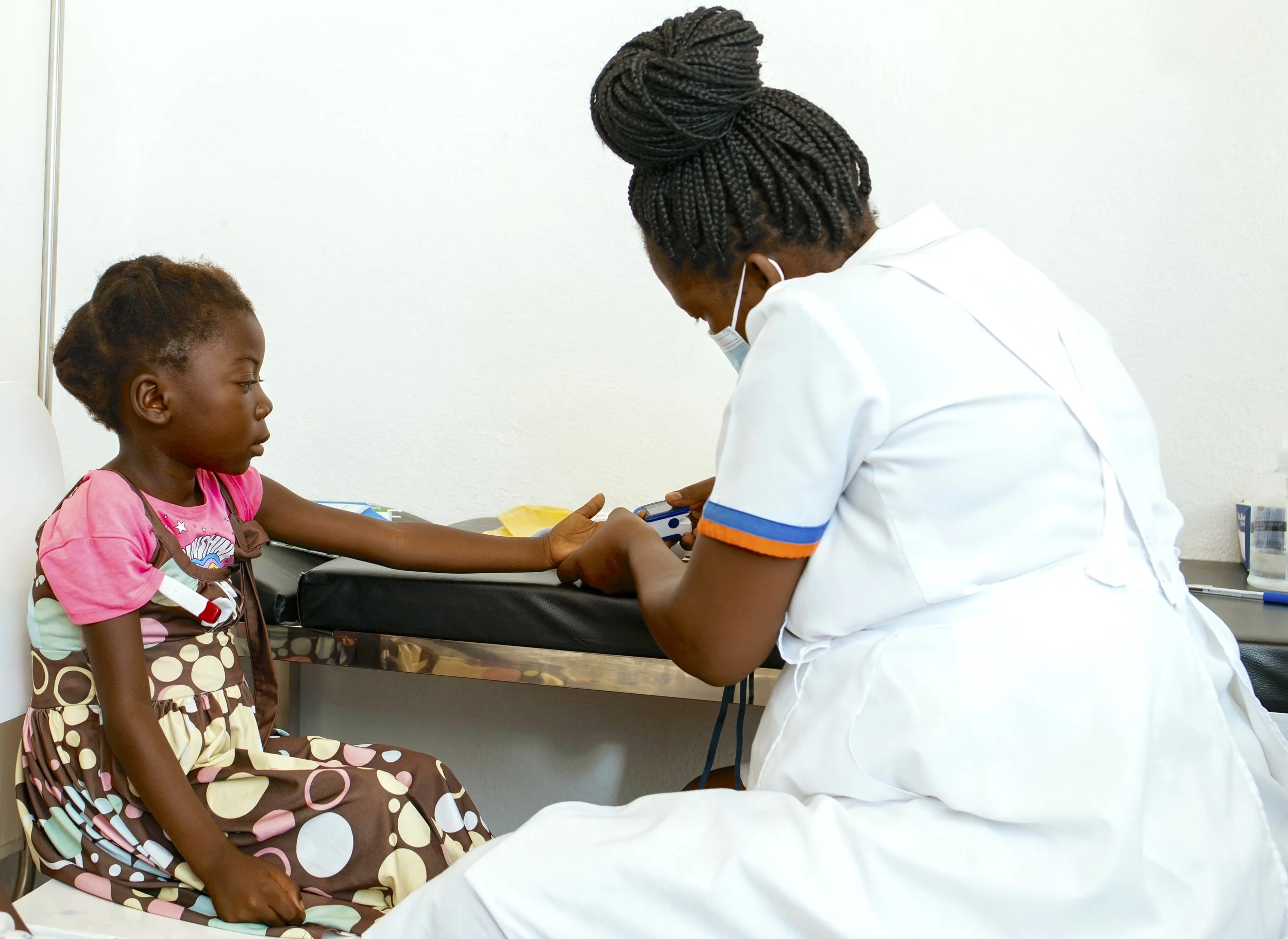
Linda receives treatment for her sickle cell disease at the PEN-Plus clinic in Nhamatanda, Mozambique. PEN-Plus, an integrated care delivery strategy designed for low-resource settings, is the most advanced example of integration science in action. (Photo: ©Ivan Simone Congolo/World Health Organization)
As global health funding continues to contract, a four-paper series being prepared for publication in The Lancet will provide the case for integration science as a tool for unlocking significant gains in health equity worldwide.
Fifty-two authors from 17 countries are writing the papers. These experts represent a range of organizations worldwide and include academics, ministry officials, and people with lived experience from across sub-Saharan Africa and South Asia.
Led by the NCDI Poverty Network’s co-chairs—Dr. Gene Bukhman, executive director of the Center for Integration Science in Global Health Equity at Brigham and Women’s Hospital in Boston, Massachusetts, and Dr. Ana Mocumbi, an associate professor at Universidade Eduardo Mondlane in Maputo, Mozambique—the series will present both the theoretical framework and real-world applications of integration science for global health equity.
A relatively new field, integration science offers a systematic approach to increasing the resources available to people worldwide across steep gradients of inequality. Integration science accomplishes this goal by aligning health workforce capabilities and clinical pathways with the needs and shared experiences of those directly affected by disease.
“We’ve been seeing countries independently moving toward integrated care delivery out of necessity, but these efforts are often fragmented and narrow,” said Dr. Bukhman, lead author of the series and a professor at Harvard Medical School. “Integration science provides a data-driven methodology to make these efforts more comprehensive and effective. And, when you combine integrated delivery models with integrated social movements, you create the conditions for real progress in global health equity.”
The research captured in the series draws from a dataset of more than 5,000 patient observations in dozens of healthcare facilities across sub-Saharan Africa and South Asia. Through extensive patient shadowing and direct observation, researchers have documented the details of clinical resources, competencies, and care pathways that form the foundation for integration science applications.
The first paper will review lessons from the first five years of the NCDI Poverty Network, an initiative launched in 2020 to implement the recommendations of the Lancet Commission on Reframing Noncommunicable Diseases and Injuries for the Poorest Billion. The Network already includes 29 countries, 16 of which are implementing PEN-Plus, an integrated care delivery strategy designed for low-resource settings.
The second paper will introduce a four-step process that helps health systems move from fragmented care to integrated approaches. Through case studies, this paper will demonstrate how countries can systematically use this delivery model design to assess existing capacities, identify integration opportunities, and reconfigure care pathways for maximum efficiency.
Paper three proposes moving beyond traditional advocacy categories—whether disease-specific, demographic, or health system–focused—toward integrated social movements based on the shared experience of illness.
The final paper will present detailed case studies to demonstrate how integration science can inform national health planning and resource allocation decisions. The authors hope the paper’s insights will help inform the broader conversation on global health allocations.
“Integration science offers a path forward for low- and lower-middle-income countries grappling with growing disease burdens and constrained resources,” said Dr. Mocumbi, who also serves as chief of the Non-Communicable Diseases Division of the Mozambique National Institute of Health. “By harnessing integrated delivery models and integrated social movements, this approach can help countries achieve effective, equitable health service delivery systems that provide lifesaving care for even the poorest people in remote, rural areas.”
Linda (on her mother’s lap) and older sister Sara (left foreground) have regular checkups at the PEN-Plus clinic in Nhamatanda, Mozambique, where a team of clinicians—including Dr. Lindolfo dos Santos (standing) and Dr. Charles Chale (right foreground)—guide their care for sickle cell disease. (Photo: ©Ivan Simone Congolo/World Health Organization)