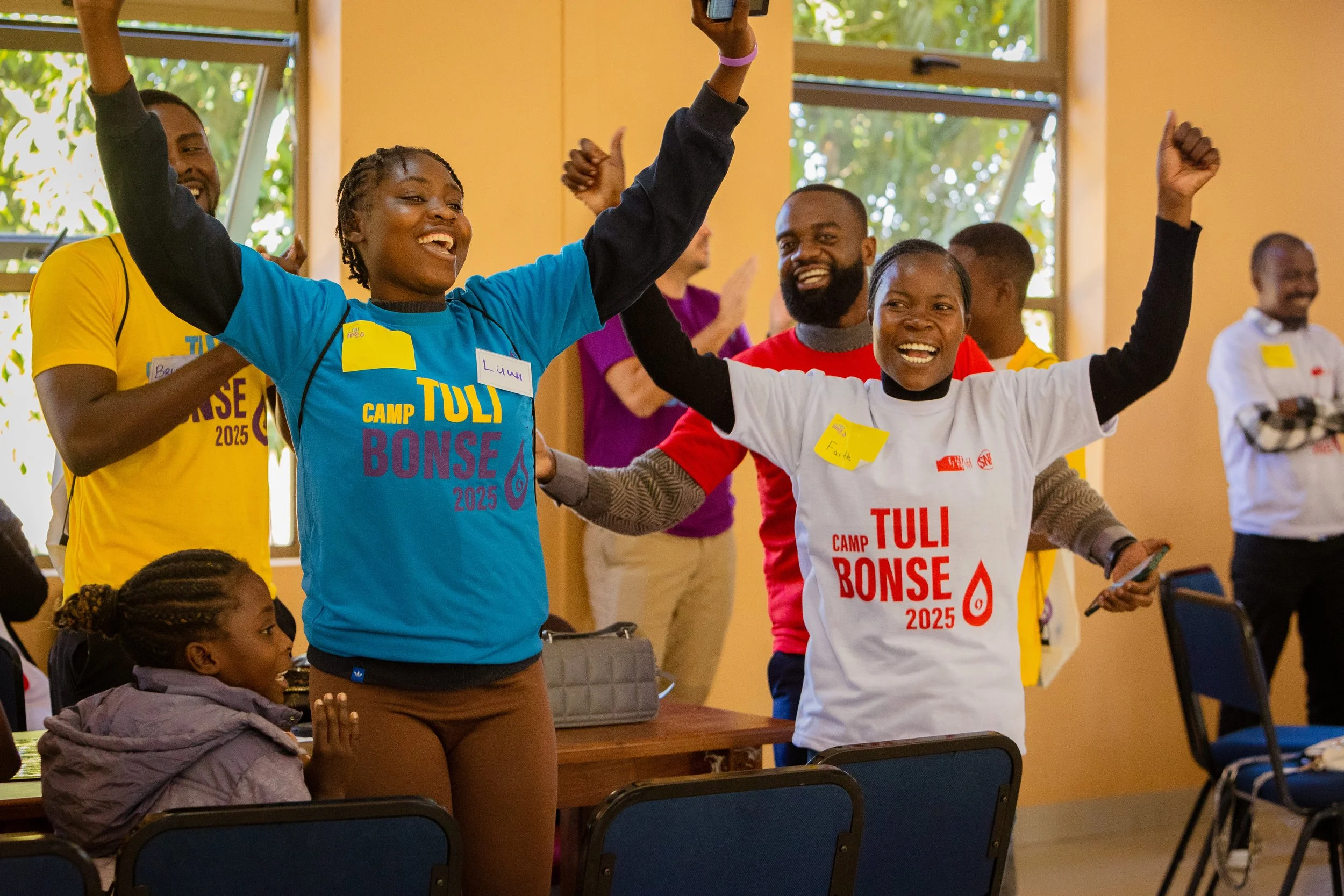Policy
The NCDI Poverty Network supports health leaders as they develop policies that prioritize equitable, cost-effective health interventions.
National NCDI Poverty Commissions—which are composed of Ministry of Health policymakers, clinicians, academic researchers, health planning and financing experts, implementing partners and donors, and people living with severe conditions—are the backbone of the NCDI Poverty Network.
The Network’s Policy Team works with National Commissions to develop policies that prioritize equitable, cost-effective interventions to address severe conditions disproportionately affecting children and young adults living in extreme poverty. In particular, the Policy Team supports National Commissions in countries that have recently joined the Network in working through the first phase of the Network’s Four-Phase Theory of Change: Situation Analysis and Priority-Setting.
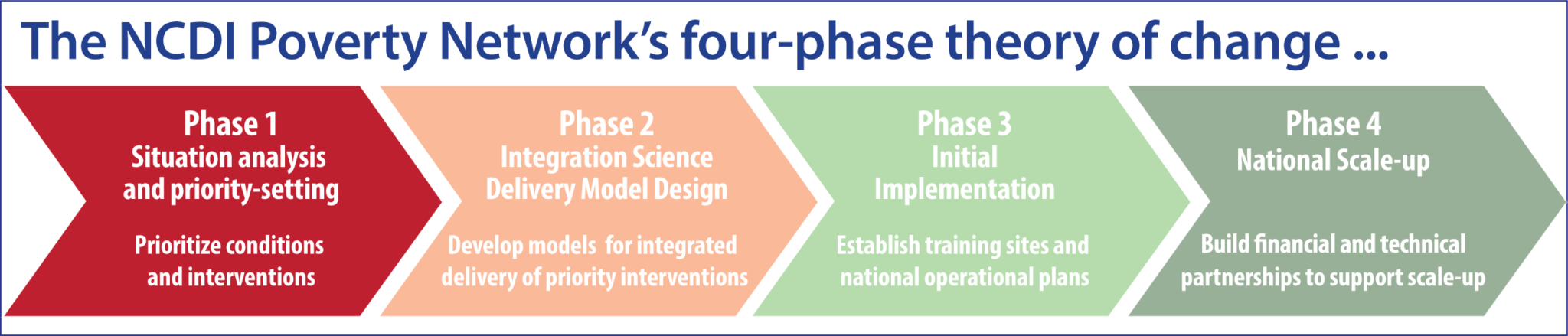
During this first phase of the Network process, National Commissions analyze the national burden of NCDs and injuries, disaggregated by age, sex, and socioeconomic status, and assess the availability and coverage of NCDI services at different levels of the health system, in order to understand disparities in prevalence, access to services, and outcomes for poor and marginalized populations. Based on findings from this situation analysis, Commissions then prioritize conditions and interventions to address the burden, taking into account both cost-effectiveness and equity, and estimate the cost and potential impact of prioritized interventions as well as the fiscal space required to implement them. Finally, Commission members disseminate their key findings and recommendations to elevate equitable access to care and treatment for severe conditions that disproportionately impact the poorest children and young adults as a priority for national policies and financing.
The Policy Team supports countries through this process by:
Sharing analytical frameworks, methods, and tools developed by the Lancet NCDI Poverty Commission, as well as a priority-setting tool developed in collaboration with the Center for Integration Science in Global Health Equity research team and the Bergen Center for Ethics in Priority-Setting;
Facilitating exchanges of experience and lessons learned with more than a dozen countries that have successfully completed this phase; and
Assisting with preparation and dissemination of reports summarizing their key findings and recommendations.
Policy and National Commission Updates
Several countries that have already implemented PEN-Plus are now launching national operational plans to detail how they will use the model to expand, integrate, and decentralize care for people living with noncommunicable diseases. A leader in Kenya’s Ministry of Health recently revealed critical steps in ensuring that country’s plan would be a success.
A recent training session showed that skills such as mentoring, proficiency in giving effective feedback, and being able to assess patient experiences accurately can be as vital to quality care as medical equipment and resources.
The clinics at Mfou and Djoum district hospitals arose from years of collaboration driven by Cameroon’s Ministry of Health and the WHO Regional Office for Africa, with boosts from an informal coalition of health officials in Francophone countries.
The NCDI Poverty Network joined with the Government of Ethiopia, the Mathiwos Wondu Foundation, the World Health Organization, and other partners in a recent ceremony to launch Ethiopia’s PEN-Plus National Operational Plan, marking another major milestone for the growth of PEN-Plus in sub-Saharan Africa.
With peer support having proved to be a key component of PEN-Plus care, the NCDI Poverty Network is developing an integrated training program for peer educators. “We’ve seen beautiful examples of young people who are unafraid to speak boldly about their condition, to be advocates, to be champions,” said Dr. Colin Pfaff, the Network’s associate director of programs. “They are living successful lives and are examples to others, which has such a powerful impact.”
A recently published study found that patient education and peer support helped people living with type 1 diabetes in rural Liberia manage their disease. “Their extra barriers to health,” said Dr. Alma Adler, the Network’s research director, “make it even more critical for patients in low-resource settings to gain both problem-solving skills and a strong clinical understanding of their condition.”
For several years, without funds for transportation or food, Yismaw Nigussie, a 15-year-old living in rural northern Ethiopia, would risk his health even getting to the clinic that provided treatment for his type 1 diabetes. Then a routine assessment changed the trajectory of his life.
Five years. Twenty-nine countries. Over a hundred PEN-Plus clinics. More than 30,000 patients. Together, the many collaborators that compose the NCDI Poverty Network deliver hope and healthcare to children, adolescents, and young adults navigating the dual challenges of poverty and severe, chronic noncommunicable diseases. And this is just the beginning.
The catchy, R&B-style track is providing new support and empowerment for people living with severe, chronic noncommunicable diseases such as type 1 diabetes.
The Kenya Ministry of Health, NCD Alliance Kenya, NCDI Poverty Network, and partners convened for Kenya’s inaugural National NCD Conference, which featured the launch of a PEN-Plus National Operational Plan.
A new initiative to strengthen global collaboration and research on noncommunicable disease care in low- and middle-income countries marks “an important milestone for scientific cooperation between Europe and Africa.”
The October tour showed the strong work of a relatively young PEN-Plus program that is poised for growth, reflecting the adaptability of the integrated model of care for noncommunicable diseases.
The same week that global policy talks on noncommunicable diseases were taking place at the United Nations General Assembly in New York City, health leaders in Abuja, Nigeria, were marking progress in being able to provide care for people living with severe, chronic NCDs through PEN-Plus.
During the opening plenary of the Sept. 25 High-Level Meeting on NCDs and Mental Health, at the UN General Assembly in New York City, repeated mentions of PEN-Plus as a successful strategy for addressing NCDs formed a show of unity in a week often noted for dissension.
A commentary authored by Network and UNICEF leaders and published in August by The Lancet Child & Adolescent Health makes the case for better care for children and adolescents living with severe, chronic NCDs in settings of extreme poverty, a case that’s also reflected in the Network’s position statement ahead of the United Nations High-Level Meeting on NCDs in September.
Zambia health officials recently opened the country’s fourth and fifth PEN-Plus clinics, marking both occasions within weeks of launching the country’s national operating plan for the care of people living with severe noncommunicable diseases. Both new clinics have received support from the Scottish Government.
In a launch event in late July, the Republic of Somaliland announced a partnership with the NCDI Poverty Network to support people living with severe, chronic noncommunicable diseases through PEN-Plus. In a statement, the Ministry of Health Development of the Republic of Somaliland noted the partnership “marks a significant step forward in strengthening the ministry’s efforts to improve health services, particularly in addressing noncommunicable diseases.”
The second International Conference on PEN-Plus in Africa positioned Nigeria as a leading advocate for PEN-Plus across the African continent, media coverage of the July conference showed.
Zambia health officials recently took a significant step forward in PEN-Plus implementation with the launch of a national operational plan to support and expand care for people living with severe, chronic noncommunicable diseases. The Centre for Infectious Disease Research in Zambia, or CIDRZ, a PEN-Plus implementing partner working with the NCDI Poverty Network, hosted a launch event in Lusaka.
Dr. Ana Mocumbi, co-chair of the NCDI Poverty Network, recently received the Republic of Mozambique’s Medal of Merit for Science and Technology. The honor recognizes her outstanding contributions to science, technology, and innovation in Mozambique.
Health officials from several French-speaking countries in western and central Africa have begun meeting in a new webinar series to share—in French—their challenges and successes in expanding care for people living with severe noncommunicable diseases. The new series solidifies a groundbreaking collaboration that began with a February study tour in Sierra Leone.
On behalf of the NCDI Poverty Network, Rachel Gasana, senior director of advancement, testified at the multistakeholder hearing on noncommunicable diseases, held at the United Nations Headquarters in New York City. The Network was one of 70 organizations selected to deliver testimonies as a prelude to the United Nations High-Level Meeting on NCDs in September.
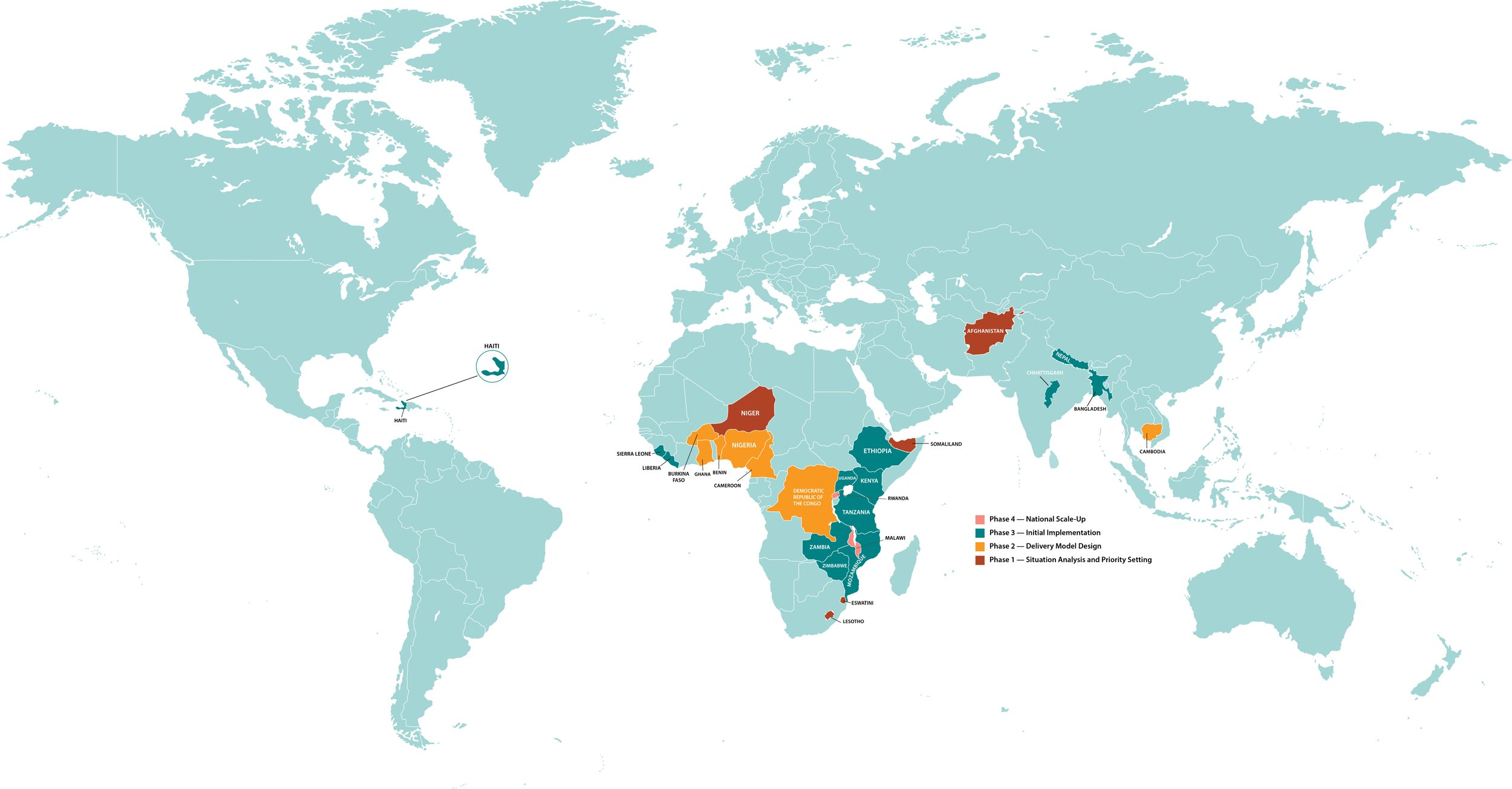
In just the past several months, the NCDI Poverty Network has grown from 23 partner countries to 27, with the most recent additions being Eswatini, Lesotho, Niger, and Somaliland.
An audience of patients, clinicians, Ministry of Health officials, and community members recently gathered to celebrate a historic milestone for Sierra Leone: the launch of a purpose-built PEN-Plus clinic at Koidu Government Hospital. Partners In Health, the implementing partner for PEN-Plus in Koidu, has published an account of the clinic’s services.
The NCDI Poverty Network has submitted proposals to the World Health Organization suggesting it add analogue insulins and a triple fixed-dose antihypertensive medicine combination to its Model List of Essential Medicines. The Network has also proposed that WHO reclassify hemoglobinopathies to shine more of a spotlight on sickle cell disease and thalassemias.
The WHO Regional Office for Africa recently published a landmark report that details the impact and momentum of the PEN-Plus model, providing a valuable tool for advocacy and information about integrated care for people living with severe, chronic noncommunicable diseases.